Respiratory Infections
Respiratory infections are common in cats, especially in high-density populations such as shelters, breeding catteries, and feral cat colonies. A variety of viruses, bacteria, fungi, and protozoa cause these infections, which negatively impact feline health. While vaccines have greatly reduced the incidence of serious respiratory disease in cats, they have not eliminated the highly contagious pathogens that cause them.
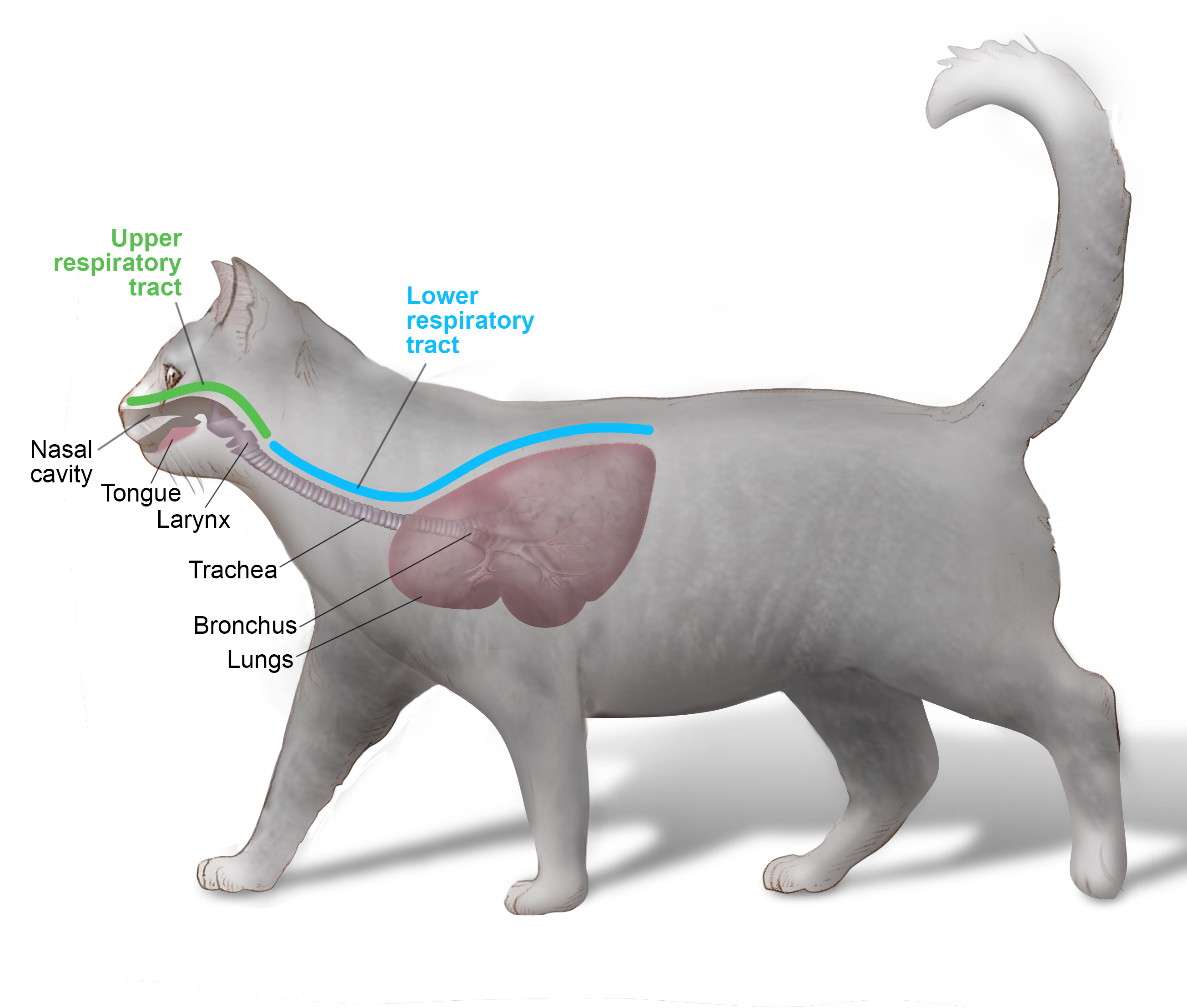
Infections can occur in the upper and lower regions of the respiratory tract. The upper respiratory tract includes the nasal passages, sinuses, oral cavity, back of the oral and nasal cavity (pharynx), and the vocal folds (larynx). The lower respiratory tract includes the trachea, bronchi, and lungs (see Figure 1).
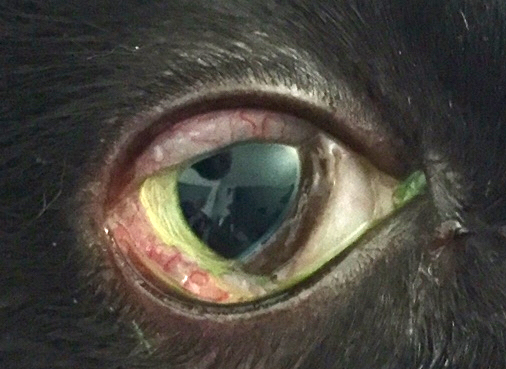
Symptoms of upper respiratory tract infections include clear or colored discharge from the eyes or nose, coughing, sneezing, swelling of the mucous membranes around the eyes (conjunctivitis, see Figure 2), ulcers in the mouth, lethargy, and anorexia. In rare cases, cats may have trouble breathing.
Lower respiratory tract infections may cause coughing, lethargy, anorexia, and difficult or rapid breathing (which should not exceed 35 breaths per minute at rest).
FELINE HERPES VIRUS
Young and adolescent cats are most susceptible to this common infection. Up to 97% of cats are exposed to feline herpes virus in their lifetime, and the virus causes a lifelong infection in up to 80% of exposed cats. Of these, up to 45% will periodically shed the virus, usually when stressed.
Clinical Signs
Commonly referred to as feline viral rhinotracheitis (FVR), herpes infection can cause upper respiratory signs (see third paragraph above), ulcers on the cornea (keratitis), and fever.
Diagnosis
FVR is usually diagnosed by recognizing upper respiratory signs in young or unvaccinated cats, or recurring conjunctivitis or keratitis in older cats, combined with the results of various diagnostic tests. These tests include polymerase chain reaction (PCR), which identifies viral DNA, and virus isolation tests that detect herpes by culturing the virus from clinical samples.
Treatment
Multiple factors, including the severity of disease, are considered when deciding the best treatment for FVR. In all cases, appropriate supportive care, such as maintaining adequate nutrition and hydration, is very important. Nasal decongestants may be helpful in some cases. It is important to note that the stress of giving medications may worsen bouts of keratitis and conjunctivitis that may otherwise subside on their own.
In acute cases of infection in young cats, antiviral drugs may help treat lesions on the cornea and upper respiratory signs. Systemic antibiotics can also be used to control the secondary bacterial infections that commonly occur with FVR. Recurring cases of keratitis or conjunctivitis can often be managed with antivirals, drugs such as corticosteroids, and by limiting stress caused by crowded living conditions, surgeries, the introduction of new cats, or moving. While lysine supplementation is sometimes recommended, this treatment is quite controversial. Several studies suggest that lysine supplementation is not effective and may actually worsen symptoms and promote shedding of the virus.
Prognosis
Once infected, cats carry the infection for life and may experience recurring bouts of upper respiratory and eye disease. While these flare-ups are often relatively mild and clear up on their own, infections can, in rare cases, lead to more significant illness and even death in cats with coexisting health problems.
Prevention
Vaccination against feline herpes is recommended for all cats. Although current vaccines do not prevent infection in all cases, they significantly decrease the severity of disease and the shedding of virus. This is beneficial to other susceptible cats, particularly those living with the cat being vaccinated.
FELINE CALICIVIRUS
Feline calicivirus is a highly contagious and common virus in cat populations worldwide. Approximately 10% of cats housed in small groups are infected, while up to 90% of those housed in more crowded conditions, such as in shelters and breeding catteries, may be infected.
Clinical Signs
While most cats infected with calicivirus develop upper respiratory signs (see third paragraph above), the infection may spread to the lower respiratory tract and cause pneumonia. Viral pneumonia may be exacerbated by secondary bacterial infections of the lungs, resulting in increased difficulty breathing. In rare cases, susceptible cats may develop inflammation or ulcers in the mouth. Even more rarely, the more severe systemic form of the disease occurs. This form is fatal in approximately two-thirds of affected cats. Systemic calicivirus often causes swelling of the head and limbs and crusting sores and hair loss on the nose, eyes, ears, and footpads. Additionally, the mouth and ears may become yellowish (jaundiced) due to liver damage, and cats may experience bleeding in the gastrointestinal tract and under the skin. In rare cases, cats may experience temporary limping when infected or after receiving a calicivirus vaccine.
Diagnosis
If oral ulcers and signs of acute upper respiratory disease cause a veterinarian to suspect calicivirus infection, the diagnosis can be confirmed by a technique called reverse transcriptase polymerase chain reaction (RT-PCR), which can detect the genetic material of calicivirus in blood samples or from swabs taken from the mouth or eyelids. Growing calicivirus from clinical samples in the lab also confirms the diagnosis.
Treatment
Supportive care, including assurance of adequate hydration and nutrition, is vital. This may be challenging, as painful lesions in the mouth may make eating and drinking uncomfortable, and congested nasal passages can block the perception of food odors that stimulate the appetite. Non-steroidal anti-inflammatory drugs can minimize oral pain, and the nasal passages should be cleared using drugs to break down mucous, nebulization with saline, and regular wiping with a saline solution. A feeding tube that bypasses the oral cavity may be recommended until oral lesions subside.
Antibiotics may be used to combat secondary bacterial infections in the mouth and respiratory tract. Unfortunately, available antiviral drugs are either ineffective or have significant side effects in cats. While some cats with severe systemic calicivirus infection have been reported to improve when given a combination of corticosteroids and interferon, the safety and effectiveness of this therapy needs more thorough testing before it can be routinely recommended.
Veterinarians may recommend that cats with chronic oral ulcers receive rigorous dental cleaning, combined with immune-modulating drugs, antibiotics, and pain-relieving medications, but controlled studies to determine the best treatment for this aspect of calicivirus infection are still needed.
Prognosis
The prognosis for cats with calicivirus infections depends upon the severity of symptoms. Cats with uncomplicated upper respiratory disease, pneumonia, or oral ulcers may recover in days or weeks, while those with severe systemic disease have a much less favorable prognosis.
Prevention
Vaccination against feline calicivirus is recommended for all healthy cats. Although the vaccine is not 100% protective, it does reduce the likelihood of severe disease. Vaccines do not, however, prevent shedding of this ubiquitous virus or cure cats that are already infected.
FELINE CHLAMYDIOSIS
Chlamydia felis is a bacterium that cannot survive outside of its host and therefore requires close contact between cats for transmission. Transmission occurs through eye secretions. Infections occur most commonly in young cats and in cats housed at high density in shelters and breeding catteries. Approximately 20% of cats with upper respiratory signs and about 3% of healthy-looking cats carry C. felis.
Clinical Signs
Infected cats usually develop conjunctivitis with eye discharge that is initially clear, but later contains mucous and has a yellowish, pus-like appearance. Rarely, infected cats lose their appetite and become lethargic.
Diagnosis
The preferred method of verifying infection is the use of PCR to identify C. felis DNA from eye swabs. The organism can also be grown in the lab, but this technique is not as sensitive as PCR. Unvaccinated cats can also be tested for C. felis antibodies.
Treatment
Antibiotics (e.g. doxycycline, amoxicillin/clavulanic acid) are generally effective in treating chlamydiosis in cats, with systemic treatment being more effective than topical application to the eye.
Prognosis
The prognosis for infected cats that are appropriately diagnosed and treated is generally good.
Prevention
While vaccines are available, they do not prevent infection, but rather minimize the symptoms. Vaccination is recommended for cats in multi-cat housing situations and those in which C. felis has previously been diagnosed.
FUNGAL INFECTIONS
A number of fungal species can cause respiratory disease in cats. The most common is Cryptococcus neoformans. Cats contract C. neoformans when they inhale fungal spores. The infection may remain within the nasal cavity or spread to other parts of the body, including the central nervous system and the lower respiratory tract. This organism is pervasive, and approximately 4% of all cats are asymptomatic carriers. Cats are approximately six times more likely to develop disease after exposure than dogs, and cats of all ages are equally susceptible. Bird droppings and decaying plant matter provide an ideal environment for C. neoformans and may be sources of infection. Pigeons are frequent carriers. A closely related fungus, Cryptococcus gattii, causes very similar disease symptoms.
Clinical Signs
C. neoformans infections most commonly occur in the nasal form, in which cats develop nasal or facial swelling, sneezing, chronic nasal discharge that may become bloody, and, ultimately, wounds that won’t heal or fleshy polyp-like growths in the nose and throat. Affected cats may demonstrate changes in the tone of their vocalizations, and noisy breathing and snoring. They may also become anorexic and lose weight. If the infection spreads to the lungs, affected cats may demonstrate labored or rapid breathing. C. neoformans infections can also affect the central nervous system and the skin, and in rare cases may become systemic and spread to multiple organs or systems in the body.
Diagnosis
The preferred method of diagnosis is identification of C. neoformans proteins in body fluids, ideally blood. Examining fluid samples, such as nasal discharge, under a microscope (cytology) can also be helpful, as C. neoformans has a characteristic microscopic appearance. X-rays, CT scan, or MRI may be recommended to determine how deeply the fungus has invaded the bony structures in the nose and sinuses and to monitor the response to therapy.
Treatment
While a number of anti-fungal drugs are used to treat C. neoformans infections, definitive guidelines regarding which should be used in specific cases are lacking. In some cases, spread of infection to certain organs, such as the brain, may alter therapeutic recommendations and outcome.
Prognosis
The prognosis for cases diagnosed early in the disease and with no involvement of the central nervous system is generally favorable. One major factor influencing outcomes is compliance with therapy, which may last months to years.
Prevention
Since outdoor cats are exposed to C. neoformans more frequently, keeping cats indoors minimizes the risk of infection.
OTHER FUNGI
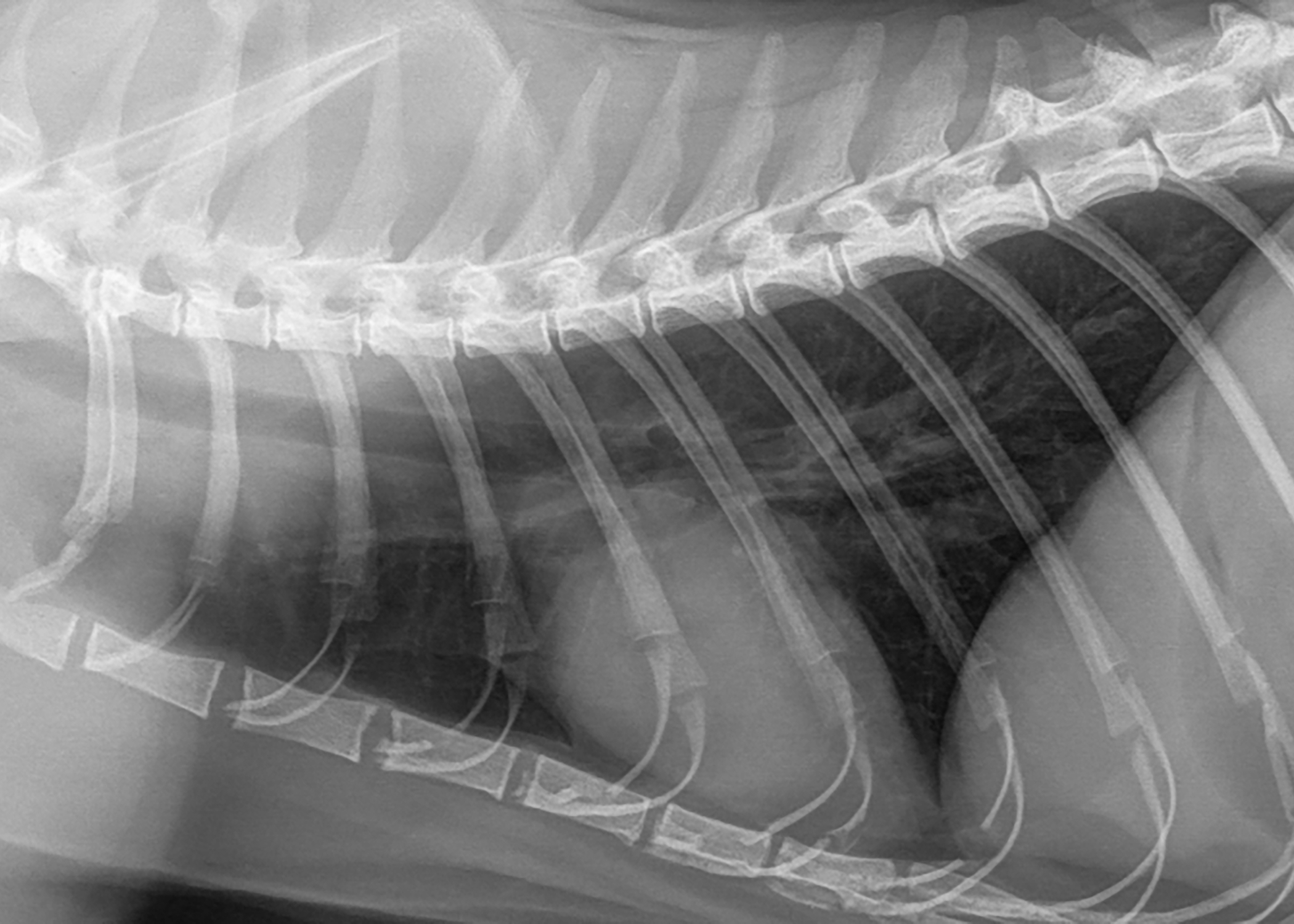
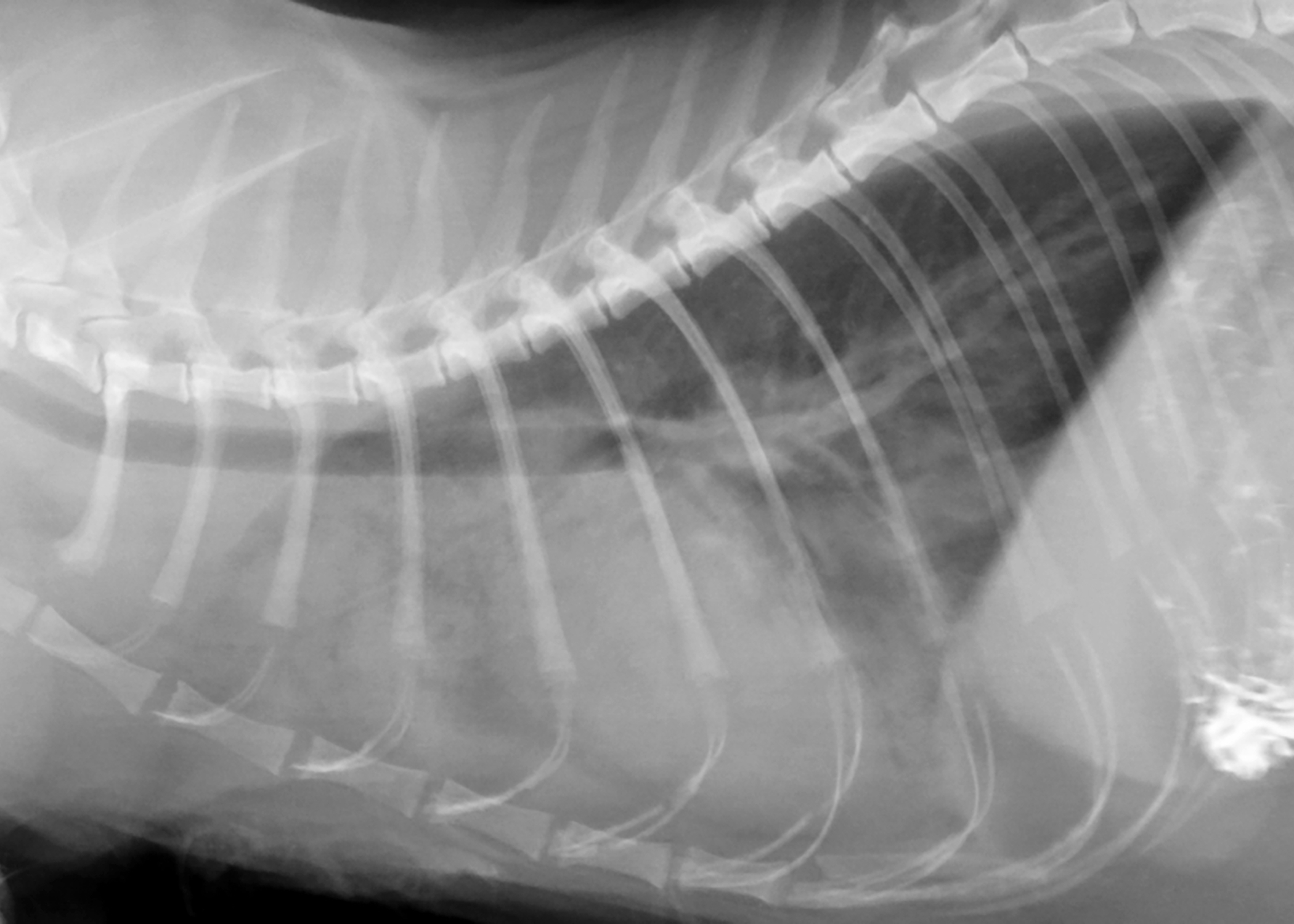
A number of other fungi cause respiratory infections in cats, including Aspergillus fumigatus, Histoplasma capsulatum, and Blastomyces dermatiditis. Unlike C. neoformans infections, these organisms commonly spread to the lungs of affected cats, causing pneumonia (see Figure 3) and difficulty breathing.
BORDETELLA BRONCHISEPTICA
B. bronchiseptica is a bacterium that commonly causes infections of the upper respiratory tract of cats housed in high-density populations, such as in shelters and breeding catteries. In these populations, approximately 5% of cats with signs of upper respiratory tract infections and 1.5% of cats that appear normal may harbor B. bronchiseptica. Infections spread through oral and nasal secretions, and can cause symptoms ranging from mild to life-threatening. Infected dogs may spread the bacterium to cats, and in very rare cases, B. bronchiseptica may be transmitted to people.
Clinical Signs
The clinical signs of infection vary from coughing, sneezing, and eye discharge that is mild and self-limiting to difficulty breathing, blue-tinged mucous membranes (cyanosis), and death. The more serious signs often occur in young cats that develop lower respiratory tract infections, although these may occur in older cats as well.
Diagnosis
Samples taken from the respiratory tract can be used to grow B. bronchiseptica in the lab, or to detect B. bronchiseptica genetic material through PCR. Both of these tests, however, may give negative results in infected cats.
Treatment
Antibiotic therapy (usually doxycycline) is the mainstay of therapy, although supportive care, including assurance of adequate nutrition and hydration, are very important in managing B. bronchiseptica infection in cats. Even in cases with mild symptoms, antibiotics may be recommended to prevent a worsening of the infection.
Prognosis
Most cats with uncomplicated B. bronchiseptica infections recover within 10 days of beginning antibiotic therapy. Without appropriate treatment, the disease may progress to varying degrees, from worsening upper respiratory signs to life-threatening pneumonia.
Prevention
A nasal vaccine is available, and while it is not considered a core vaccine for all cats, it should be considered for cats entering high-density housing situations. It should never be administered to cats younger than four weeks, or to cats receiving or scheduled to receive antibiotics. The vaccine may cause mild upper respiratory signs in some cats.
OTHER INFECTIONS
A variety of other organisms can cause respiratory infections in cats, including some avian and canine influenza viruses, which cats can contract from humans and dogs, respectively. Avian influenza may also be transmitted from cats to humans. Other infectious organisms include Yersinia pestis (cause of the “Great Plague”), a bacterium found primarily in rodents in the southwest U.S. that is transmitted by fleas and is potentially transmissible to humans; Toxoplasma gondii, a protozoan found in many cats that can spread to humans; and Pasteurella multocida, a normal bacteria of the feline respiratory system that may cause secondary infections.
Updated June 2018